There is something uncomfortable about the Battle of Vega
Real. If one accepts the accounts of Bartolomé de las
Casas and Ferdinand Columbus, it should be listed as the first major
battle between Europeans and Indigenous Americans, with the victory going to
the former while sending the latter into ignominious defeat and wretched
subservience. Yet the nearly mythological descriptions of the battle, with two hundred twenty Spaniards defeating a hundred
thousand Tainos seems so exaggerated as to make one wonder if it is even
possible to discover what really happened on the plain of Vega Real in March
1495. The fact Columbus had twenty
men on horse, twenty dogs, and European weapons hardly seems enough to overcome
the odds, unless one assumes, as las Casas and F. Columbus both do, that
there was some aboriginal incomprehension about what they were encountering in
arms, animals, and men, some cowardice bred of the shock of the unknown that
infected an immense gathering of people who had come from all over the island
of Hispaniola and confounded their ability to respond effectively.
In response to my article about the dogs Columbus used at
the Battle of Vega Real, I received some emails from readers who questioned why
they had not heard more the battle itself, let alone the horses and dogs that
seemed a factor in the Spanish victory. “A battle that supposedly involved 100,000
indigenous men in 1495 would seem to have been a very important battle. Why haven’t I heard of it?” Something of the
same question was in the back of my mind from the very beginning of my research
into the battle. Let me see if I can add some perspective to this very valid
question.
What Did Warfare Mean to the Indigenous of Hispaniola?
Given that the Battle of Vega Real was one of the first
military encounters between the Indigenous and the Spanish, we must consider
what warfare meant to the Indigenous of Hispaniola in 1495. Herrera’s frontispiece, reproduced in the prior blog and my article,
portrays two armies at the beginning of a field battle, each on one side of the
battlefield, weapons raised, dogs being released, cavalry entering from the
side. Would the forces gathered by Caonabo or his brother be organized this
way, as if they fought under the same rules of engagement as a European army?
The illustrator of the frontispiece of the 1601
edition of Herrera’s Historia natural does show another encounter where there was not such a structure to a battle, the attack on
Navidad when Columbus was back in Spain after his first voyage. In fact, the illustrator includes two separate panels, one showing the fortress before Columbus left Hispaniola, and one showing it under attack as he returns on his second voyage (the destruction of Navidad and Columbus's return were not simultaneous but the inclusion of ships of the return fleet made the composition more dramatic). See Figure
1.
 |
|
Figure 1. Two panels from Historia general, Herrera y
Tordesillas 1601, showing (left) the founding of Navidad and (right) its
destruction. The left caption translates: The Admiral says goodbye to King
Guacanagari, building La Navidad. The wrecked Santa Maria, from whose timbers
the fortress of Navidad was built, is shown partially sunken in the water
beside the fortress. Guacanagari, who
controlled the area of the construction, is being carried by his subjects while
Columbus surveys the area. The right
caption translates: The Admiral returned and found the tower of Navidad burned
and the Castilians murdered. The Indigenous are shown attacking with arrows and
fire.
|
As to the Battle of Vega Real in 1495, Ferdinand Columbus states that his father, understanding the
Indigenous character and habits, intended to attack the diverse multitude
scattered throughout the countryside, assaltar da diverse parti quella
moltitudine, sparsa per le campagne (Historie del S.D. Fernando Colombo,
1571, 123; Columbus and Keen 1984, 149, whose translation is less of a literal
transliteration than mine). Figueredo
(2006) describes the Tainos as giving battle “guided by strategic designs that
demanded rigid organization.” Yet Caribbean warfare was also said to be
“noisy and showy with skirmishes lasting entire days” where “a melee of
personal insults, challenges and combats was the norm” (Glazier 1978).
Thus, an alternative conception of the encounter at Vega Real might be that the Indigenous gathering on the plain did not array themselves against
the forces of Columbus, perhaps expecting a period of shouting and threats before arms were picked up. Perhaps they thought their overwhelming numbers would demonstrate their
resolve and force Columbus to retreat. Or perhaps many of them were just in their
houses and going about their lives, as they had at other times that Columbus
and his subordinates had marched through Vega Real.
Were There Military Encounters Between Europeans and
Indigenous in 1494 Before the Battle of Vega Real?
It has already been mentioned that when Columbus returned to Hispaniola in his second voyage, he found that Navidad had been destroyed and the men he left there had been killed. He was told that some of the Spaniards had fought and killed each other and the rest had been killed by the cacique Caonabo (Las Casas 1875, vol. 2, lib. 1, cap. 86, 13; Columbus and Keen 1984, 119), who would continue to be the primary Taino leader opposing Columbus during the second voyage.
Ferdinand Columbus records what appear to have been
relatively minor skirmishes in 1494 around the fortresses built for gold mining
operations (Columbus and Keen 1984, 129; Wilson 1990, “The First Skirmishes," 82-84). See
Figure 2, showing how the Indigenous were supposed to happily engage in mining and panning gold for the Spanish. They were not, however, particularly happy and manifested their displeasure quickly. An attack on the fortress at Magdelena in late 1494 brought a response that resulted in the
capture of 1,600 Indigenous in the Macoris area, 550 of whom were sent to Spain as
slaves in caravels that departed from Hispaniola on February 17, 1495 (Morison
1963, 226, translating the letter of Michele de Cuneo; Anderson-Cordova 2017, 31). Thus, there was a period where Spanish groups
building fortresses were attacked, but the resistance seems to have been rapid,
spontaneous, and not the collective effort of a group of caciques, as may have happened in March 1495.
 |
|
Figure 2. Oviedo y Valdés, Historia general, recto of leaf 66, Indigenous mining and
panning for gold. JCB Accession No. 01632, Juan de Junta, 1547, Salamanca.
|
Was the Taino Force at Vega Much Less than 100,000, Say Just 5,000?
The number of Indigenous fighters that Columbus encountered at Vega Real,
said to be 100,000 by both Las Casas and F. Columbus, is often doubted
and sometimes even summarily rejected. Antonio de Herrera y Tordesillas (1549-1625),
writing about a century after the battle, takes the number given by the earlier
sources, but rather than simply repeating that there were 100,000 Indigenous on
the plain, he hedges, saying that the natives seemed to amount to one
hundred thousand, todo el parecio ser de cien mil hombres (Historia
general, vol. 1, Decada I, lib. 2, cap. 17, 77; Parry and Keith 1984, 201).
This suggests that a sixteenth-century historian was already uncomfortable with the size
that Las Casas and F. Columbus had given the Taino force.
Kathleen Deagan and José María Cruxent (2002, 61), in their
brilliant description of the settlement at La Isabela, state that the Taino
caciques organized an insurrection, “allegedly planning to march against La
Isabela with a force more than five thousand strong,” thus ignoring the number
of combatants given by Las Casas, F. Columbus, and, grudgingly, Herrera.
A footnote in their book indicates that they have taken the more credible
number from Pietro Martire d’Anghiera’s De Orbe Novo (Parry and Keith,
1984, 208-210), which describes the force encountered in the Cibao by Alonso de
Ojeda as “about 5000 men [cinco mil hombres armados á su manera],
equipped in their fashion, that is to say, naked, armed with arrows without
iron points, clubs, and spears.” (There is probably a textual error in the 1892
edition of Martire, Fuentes historicas sobre Colon y América, which
reads, at 221, unos mil armadas instead of unos cinco mil armados).
Martire’s description of Ojeda does not
mention the Battle of Vega Real but I do believe Deagan and Cruxent have
correctly correlated the passage in Martire with events that were either part
of the Battle of Vega Real or that followed immediately after it, but I
would have liked to see further comment on this substitution of numbers. Shoring up the
accounts of Las Casas and F. Columbus by finding correlations in the accounts
of early chroniclers of the conquest who do
not specifically mention a battle at Vega Real produces a more
credible description of the battle, but such jerry rigging simultaneously demonstrates
that there is no single early account that is entirely credible. This, among
other reasons that will be discussed below, probably results in historians
shying away from paying too much attention Vega Real and makes some of them reluctant to anoint the battle as the first major
conflict between Europeans and the Indigenous.
Was the Population of Hispaniola Sufficient for an Army
of 100,000 Indigenous Even to Be Possible?
Before accepting the reduced size of Columbus’s opponents at
Vega Real, it might be appropriate to ask whether it would have even been
possible for any group of caciques to gather 100,000 people at the Vega Real in
1495. Michele de Cuneo, in a letter written in 1494, wrote that the cacique Caonabo could
field 50,000 men (Parry and Keith 1984, 89, translating from the Italian, homini
L mila; Cuneo, Lettera [1495] 1893, 99), although this reference is not
mentioned in connection with a specific battle.
A preliminary question concerns whether the population of
the island in 1495 was sufficient for such a sizeable force to be
possible. One of the first
anthropologists to estimate populations of the Caribbean was Alfred Kroeber
(1934), who placed the population of the West Indies at 200,000, meaning the
population of Hispaniola could not have fielded a force of 100,000. Angel Rosenblat (1967) put the
population of Hispaniola in 1492 at between 100,000 and 120,000, also too small.
Kroeber was attacked for his estimates. Francis Jennings
(1975, 18-19) described him as a “dissident scholar” who “emphatically
rejected the notion that the natives of North America could be considered
capable of so ordering their societies and technologies as to increase their
populations beyond a static and sparsely distributed token representation.”
William Denevan (1996) said that Kroeber’s estimates were the result of
“antithetical conceptions of the quality and capacity of aboriginal cultures
everywhere in the Americas.”
Tink Tinker and Mark Freeland (2008) estimated that the
population of Hispaniola in 1492 was just shy of eight million (7,975,000 to be
precise) but accepted that Las Casas was correct in arguing for a precipitous
decline under early Spanish rule, going down to 3,770,000 by 1496, with only
500,000 surviving by 1500 and 60,000 by 1507.
Their numbers thus allow for fielding a considerable force in 1495, but probably not a few years later.
Samuel Wilson (1997) finds the number 100,000 implausible,
though he accepts that 15,000 men could have been raised in 1497 (Stone 1990,
97-102). He makes the important observation that famine and epidemics had even
five years after contact considerably reduced the population of the island.
As I noted in my paper, recent genetics research (Fernandes
et al. 2020) has estimated that the pre-contact population of Hispaniola and
Puerto Rico combined could have been at most 80,000 people. Various assumptions are made in the calculation of population sizes using genetic
analysis, but if this research is upheld, a lower number than some of those
proposed will likely have to be accepted and the estimates of Kroeber and
Rosenblat may be judged not so far off after all.
If Las Casas and F. Columbus Exaggerated the Number of
Indigenous at Vega Real, Why Did They Do So?
Juan Friede and Benjamin Keen (1971) summarize some of the
reasons for exaggeration of population estimates in sixteenth-century accounts
(I add numerals in brackets):
[1] The conquistadors wished to
stress the heroism of their feats; [2] the clergy sought to enhance the
importance of their missionary and evangelizing work; [3] pro-Indian
polemicists wished to present a somber picture of the activities of the
conquistadors; [4] enthusiasts of the Indians’ past were eager to idealize or
hyperbolically exalt that past; and [5] obsessive Hispanophiles wanted to
present the Indian as a biologically and culturally inferior being.
Las Casas could have exaggerated for reasons (2) and (3), F.
Columbus for (1), and modern commentators who uncritically accept the numbers
of earlier accounts may belong in (3) through (5), though laziness in questioning
earlier accounts may not implicate any serious bias due to any of these
reasons.
How Many Allies Did Columbus Bring to Vega Real?
Two hundred twenty men against 5,000, accepting an
adjustment to the numbers of Las Casas and F. Columbus, is still a significant
discrepancy and it would seem that even a terrified mass of 5,000 Indigenous
fighters could get off enough arrows to finish off a few hundred men, horses,
and dogs. As I mentioned in my paper,
the size of Guacanagari’s force allied with Columbus becomes, therefore, a
significant factor. F. Columbus assigns no number to the allied force, saying only that Guacanagari
was eager to oppress his enemies, Guacaanagari molto disderoso di opprimere
I suoi nimici (F. Columbus, Historie del S.D.
Fernando Colombo, 1571, 123; Columbus and Keen 1992, 148). Las Casas realizes that
the size of Guacanagari’s force would be relevant, but parenthetically
apologizes that he could not find the number of his vassals, (no pude saber
qué gente llevó de Guerra, de sus vasallos). (Las Casas, 1875, vol. 2, lib.
1, cap. 104, 97).
Here again, some creativity is required to estimate the size
of Guacanagari’s contribution in men. I noted in my paper that Erin Stone
(2021) takes the number of 3,000, citing Sauer (1966, 89, who only refers to
"Guacanagari of Marien and his men"). The number is, however, quite credible as it is used
by Martire for the indigenous allied force later used by Bartolomé Columbus
against Guarionex (1892, vol. 1, Decada 1, lib. 7, cap. 1, p. 284).
Who Led the Indigenous Forces against Columbus at Vega
Real?
The frontispiece panel of the 1601 edition of Antonio de
Herrera’s Historia general depicts
Columbus facing Guarionex, their respective armies behind them. Were the Battle of Vega Real such a clearcut
European-style engagement, one would expect accounts to identify the two commanding
generals that faced each other in March 1495.
This is not the case, however, and it is doubtful that we can ever be
certain who led the Indigenous forces, or whether they were even under the
command of a single individual.
Las Casas does not specifically name a commander for the
Indigenous forces, though in the chapter that describes the battle he does
refer to Guatiguana, Cacique of Magdelana, who had earlier killed ten Spaniards,
10 cristianos (Las Casas, 1875, vol. 2, lib. 1, cap. 104, 98). Wilson (1990, 89-90) notes that Samuel Eliot Morison,
in Admiral of the Ocean Sea, preferred Guatiguaná as the leader of the
resistance, a possibility Wilson does not reject though he also accepts the
possibility that the leaders were “notorious and nameless brothers of Caonabo.”
The latter would be the current author’s choice, should he be entitled to have an
opinion on this. Wilson, correctly in my
opinion, states that although Guarionex is “consistently considered by all of
the chroniclers to have been the most powerful cacique in the Vega, [he] is not
mentioned at all and seems not to have been involved.” Since Fray Ramón Pané
was sent by Columbus to live among the people of Guarionex in 1495, it is
unlikely this would have worked very well had Columbus and Guarionex been so
hostile to each other in March 1495 (Pané 1999, xxi). It could not be ruled
out that one of the caciques subordinate to Guarionex might have been important
at Vega Real (Kulstad 2008, 39, discussing Maniocatex, more often spelled Manicaotex).
Ferdinand Columbus indicates that Caonabo, frequently
described as one of the most powerful caciques of the island, was taken alive at
the battle, along with his wives and children, e preso vivo Caunabo,
principal Cacique di tutti loro, insieme co’ suoi figliuoli, & con le sue
donne (F. Columbus, Historie, 1571, 123). It perhaps should be noted
that Keen, in translating the passage, adds a footnote stating the F. Columbus
was in error in that “Caonabó neither participated in nor was made prisoner in
this battle, but was captured by Hojeda by a ruse.” (See Tyler 1988, 164, summarizing the three most common narratives of how Caonabo was captured.)
As noted above, Deagan and Cruxent cite Martire to give the
number of Columbus’s opponents at Vega Real as 5,000. Let us look at Martire’s chronicle more
closely. He notes that Columbus had
left Hispaniola in 1494 to try to reach the Far East, which he believed to be close, but
after some exploration returned only to learn that Caonabo was besieging Alonso de Ojeda at the
blockhouse of Santo Tomás. Martire says Caonabo would not have begun such a siege had he known that Columbus himself was coming with imposing
reinforcements, no habían levantado el sitio hasta que vieron que venía el
mismo Almirante con gran escuadrón (Martire 1892, vol. 1, Decada 1,
lib. 4, cap. 1, 208; Parry and Keith 1984, vol..2, 208). Martire
says that Caonabo was encouraged by other caciques to expel the Spanish.
Caonabo then left with a large force, probably to attack Columbus, but Ojeda separated
the cacique from his men and brought him to Columbus, where he was seized
and put in irons, fué preso y encadenado (Martire, 210; Parry and Keith,
209).
Martire continues that, after the capture of Caonabo,
Columbus resolved to march throughout the whole island, determinó recorrer
las isla (Martire 1892, cap. 2, 211; Parry and Keith 1984, 209). After a
long passage concerning the Spanish search for gold in Hispaniola, Martire returns
to the events concerning Caonabo, now in irons. Martire states that Caonabo
pleaded with Columbus to protect his territory, which was being ravaged by his
native enemies in his absence. His real purpose, however, was to lay a trap for
Columbus because Caonabo’s brother had assembled five thousand men to attack
the Spanish. Ojeda, however, decided to go on the attack rather
than wait to be attacked and, finding the ground well adapted for cavalry
maneuvers, his horsemen rode down the enemy, who died if they remained in place.
Only those who abandoned their houses for the mountains and rough cliffs
survived, abandonando sus casas se refugiaron en las montañas y en ásperos
riscos (Martire 1892, cap. 4, 222; Parry and Keith 1984, 211).
This passage from Martire, which I believe ends with a
description of an encounter that was either part of the Battle of Vega Real or followed soon after, does not conform with Las Casas or F. Columbus in that Columbus
himself is not present, but it agrees with them in stating
that cavalry was essential in the victory, though dogs are not mentioned.
It may also give a clue about the type of fighting that was occurring at
this time in that the natives that awaited the battle in their houses were
killed, whereas those who fled might survive. Does this mean that some of the
“battles” described involved not an open field of battle but something closer to the
attacks of the U.S. Army against defenseless villages in the nineteenth century plains warfare? Perhaps David Traboulay (1994, 26) is correct in arguing that when Columbus, his brother Bartholomé, and Ojeda "took a series of military expeditions all over the island," they were specifically attacking villages that could not pay the tribute Columbus was imposing.
Oviedo (1851, vol. 1, lib. 3, cap. 1, 59) also describes
Caonabo’s siege of Santo Tomás, in territory under his control, which involved
assembling archers to attack the fort and burn it. Ojeda, as in Martire’s
account, captured Caonabo, but Caonabo’s brother, who was well respected by the
Indigenous (hombre de mucho esfuerço quisto de los Indios) then gathered
a force of seven thousand men, most of them archers, and began fighting to free
his brother. Oviedo also describes the
panic that men on horseback caused among the Indigenous. Ojeda received an additional three hundred
men from Bartolomé Columbus and captured Caonabo’s brother. Later, according to
Oviedo, the focus of the opposition to the Spanish shifted to Guarionex, who
was able to gather fifteen thousand men (Oviedo 1851, cap. 2, 60), whom
Bartolomé Columbus attacked in a night battle in which he captured Guarionex in
1497 (Wilson 1990, 98).
Can the Accounts of Martire and Oviedo Be Correlated with
Those of Las Casas and F. Columbus?
Samuel Wilson (1990, 90) argued that the Battle of Vega Real
“was such a rout that Martyr does not even mention it.” Martire did, however,
mention Columbus’s desire to march across the island and also described
actions conducted by Columbus’s subordinates that may well have been part of
the overall plan that probably began with the Battle of Vega Real. It is not
clear to me why Martire would not want to mention a rout, as Wilson
argues. Another possible explanation is that perhaps the initial attack of Columbus and Guacanagari and
their forces was not a battle where their enemies were engaged and soundly
defeated on a battlefield, but rather a rampage through the villages and fields
of the northern Vega Real with only gradually developing resistance from the
inhabitants. Perhaps the soldiers from
whom Las Casas and F. Columbus received their information had altered
memory in such a way as to make the encounters into a single battle of which
they could be proud, rather than a rampage that Oviedo and Martire preferred to
ignore.
Carl Sauer (1966, 88-89) takes his summary description
primarily from F. Columbus, but curiously adds, “This was no proud conquest,
nor was it called such. The easy submission was entitled ‘pacification.’” This
would be a questionable judgment if one were to focus on the accounts of Las
Casas and F. Columbus, which were described as victories against considerable odds, but it is more easily accepted if passages from Oviedo
and Martire that probably relate to the same period are allowed to add a caution
as to how confined geographically or limited temporally the battle was. It might be expected that Martire would have incorporated the account of F. Columbus, given that he knew Fernando as a boy at the royal court and probably tutored him. (Perez Fernandez and Wilson-Lee 2021, 8).
Obviously, the inability to identify a single or specific
set of leaders of the Indigenous at Vega Real makes it difficult to imagine
the battle, and the problems in correlating the accounts of Las Casas and F.
Columbus with accounts of probably the same period by Martire and Oviedo,
undermine any faith that a definitive history of the conflicts of 1495 is even
possible.
Where Did the Battle of Vega Real Occur?
Another problem concerns the location of the battle. Ferdinand Columbus says that Columbus encountered the
scattered Indian horde two days’ march from Isabela, due gionate lungi dalla
Isabella (Historie 1571, 123; Columbus and Keen 1984, 149, at least in the 1992 edition,
incorrectly translates as a ten days’ march). Las Casas says that the
Columbus’s march from La Isabela was ten leagues, diez leguas,
from La Isabela (Las Casas, vol. 2, lib. 1, cap. 104, 97).
If one is to argue that the events around a siege of Santo Tomás
described by Martire and Oviedo contain some of the circumstances that are
attributed to the Battle of Vega Real, then it is to be noted that this would require some interval for the theater of war to move south. According to the letter of Michele de Cuneo,
who was at the fortress at Santo Tomás when it was built was built, it was about 27
leagues from La Isabela and only about two leagues from where Caonabo lived
(Parry and Keith 1984, 88-92, translation of the letter).
That the Spanish would want to fight within an easy distance
of a fortress is not in doubt. Martire (Decada 1, lib. 4, cap. 2, p 212-13)
says a number of refuges, número los refugios, were added so that they
could be reached quickly in case some violence from the islanders might
threaten the Spanish, por si acaso alguna vez les amenazaba alguna violencia
de los insulares. This would indicate that having encountered hostility,
groups of Spanish men might need a place where they could shelter and perhaps
force some acceptable sense of engagement on the natives, rather than just
enduring sporadic and random attacks.
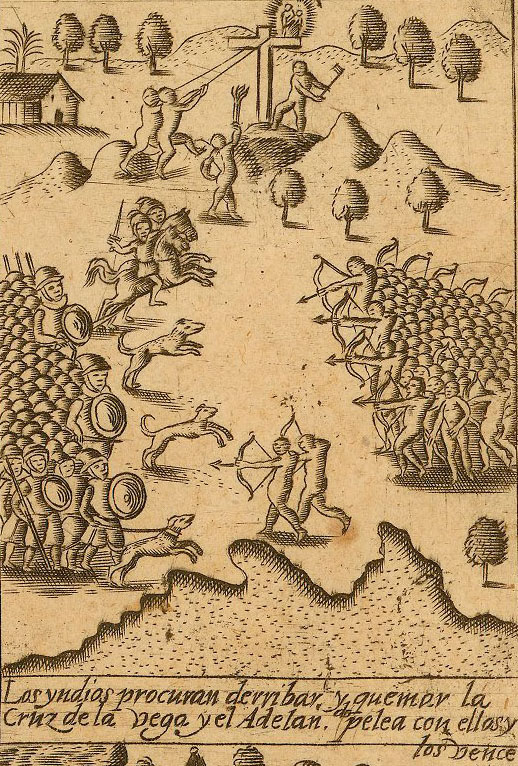
The frontispiece of Antonio de Herrera’s 1601 edition of Historia
general depicts an attempt by los yndios to destroy la Cruz de la
Vega, which is being defended by Bartolomé Colon, referred to in the
caption as el Adelantado, a title given him by his brother Christopher.
Whether this was part of the Battle of Vega Real or totally unrelated has long been
a subject of historical dispute. A particularly detailed
paper by Apolinair Tejera (1945) includes careful analysis of relevant passages
in Oviedo and Herrera, which refer to crosses erected at fortresses in
Hispaniola with little commentary. Those early accounts were expanded
novelistically, and with significant spiritual elements, by later writers.
Apolinair Tejera concluded that Herrera’s reference to
a “miracle of the Holy Cross of the Conception of La Vega” was not dated by
him, and could not be, and that the exaggerated incident of Santo Cerro must
have occurred long after the bloody disaster of Vega Real (el exajerado
incidente del Santo Cerro debió ocurrir much después del sangriento desastre de
la Vega Real). It is curious, however, that the illustrator of Herrera's book included dogs in that battle, just as he had in his depiction of the Battle of Vega Real, though the Spanish forces in the fight over the cross were under Columbus's brother, rather than Columbus. Floyd (1973) accepts
Tejera as correctly separating the incident of the cross from the Battle of
Vega Real. See Figure 3.
 |
|
Figure 3. A frontispiece panel of the 1601 edition of
Antonio de Herrera y Tordesillas’ Historia general (vol. 1) shows a
battle in defense of a cross. The
caption translates: The Indians try to tear down and burn the Cross of La Vega
and the Adelantado [Bartolomé Columbus] fights with them and defeats them, los
indios procuran derribar y quemar la Cruz de la Vega y el Adelantado pelea con
ellos y los vence. Some authors have argued this was part of the Battle of
Vega Real. Detail, John Carter Brown Library, JCB B601 H564h.
|
One recent researcher
(Stone 2021, 376) argues that upon reaching the plain of Vega Real,
Columbus and Guacanagari “set up a small palisade atop present-day Santo Cerro,
a mountain that overlooks the entire Cibao valley located in Guarionex’s
cacicazgo.” After a day of fighting, the Spaniards retreated to
Santo Cerro. Waking the next morning,
however, they were surprised to discover that the opposition forces had
disappeared in the night. This perspective on the battle conflicts with
accounts that the Tainos were put to
flight after the attack of the horses and dogs.
It also seems to accept that what is generally called the Battle of Vega
Real could as easily be called the Battle of Santo Cerro. Kulstad (2008, 41) notes that those who
distinguish the battles of Vega Real and Santo Cerro usually point out that
Santo Cerro was further from Isabela than Las Casas and F. Columbus would place
the battle. I do not think Stone adequately addresses this difficulty. Guitar (2001) also connects Santo Cerro to Vega Real but provides few references.
How Much Do We Know about the Battle of Vega Real?
The progression of events during 1495 was, I believe, something like the
following:
Angered by Spanish incursions into his territory and that of
other caciques, but seeing that isolated attacks against the Spanish only led
to defeats, Caonabo begins to assemble a force, which numbers 5,000 or more, to
push the Spanish back and perhaps to remove them from Hispaniola altogether. Guarionex
may have encouraged Caonabo to revolt, and may have been pulling strings to get
other caciques to cooperate with Caonabo, but he probably did not take any battle
leadership role until after 1495.
Columbus returns from his explorations of the Cuba and other
islands in 1494 and determines that threats to mining operations and Caonabo’s
gathering of an army require a coordinated response led by him. Caonabo is
captured by Ojeda, either by a ruse or in a skirmish. It is not impossible that F. Columbus appropriately connects his capture to the first major fighting in Vega Real. Ojeda takes Caonabo to La
Isabela, where he is kept in chains pending being sent back to Spain. A brother
of Caonabo gathers a large force, or supplements the force Caonabo has already assembled, now amounting to about 7,000 men dedicated to freeing Caonabo and continuing his crusade against the Spanish.
Beginning at the northern end of the plain of Vega Real, but
perhaps continuing near one of the defensive fortresses, Columbus, supported by
perhaps 3,000 men under his ally Guacanagari, uses cavalry and dogs and greatly
shocks the Indigenous inhabitants. Caonabo’s brother and other caciques are
taken prisoner at Vega Real or in subsequent actions. Columbus’s victory is followed by
additional battles and skirmishes led by Alonso de Ojeda and Bartolomé
Columbus, using portions of Columbus’s army. Some battles occur near the
defensive fortresses.
The encounter at Vega Real as presented by Las Casas and
F. Columbus and as depicted in the frontispiece of Herrera’s Historia
general of 1601, was a classic European battle. Although a great number of Indigenous people
had gathered at Vega Real, they may not have been organized as an army prepared
for battle but rather have been more of an intertribal gathering, assembled
to air their grievances and reach a consensus on what to do about the Spanish. They were, in any case, unprepared to respond to the organized force that began to move through them and their villages before they could even understand what
they were facing. Guacanagari would have understood that the forces of Caonabo
or his brother were not expecting what Columbus was about to deliver, and he
could have calculated how to support Columbus, making his army a significant
part of the blow that Columbus landed at Vega Real. He was assuring his own survival and probably seeking the best treatment possible for his people.
Columbus was determined to pacify the island, but he is only
mentioned as participating in the first battle that occurred after he entered
the Vega Real. He could have easily returned to La Isabela after his initial
victory and left the mopping up to Alonso de Ojeda and his brother, which
explains what Martire and Oviedo were describing. The entire island was not pacified, but the
area under Caonabo’s control probably was. Guarionex was able to mount significant resistance in 1497 (Wilson 1990,
75, 78), but was also defeated and had to flee. Columbus would have continued
to enjoy the support of Guacanagari but may have by then also incorporated some
remnants of the forces of other defeated caciques as well.
Does this perspective of the battle alter any of my findings
or opinions with regard to the use of dogs at Vega Real? Probably not. The dogs could have been chasing people who were already panic-stricken and might have
had to bite them more at the side than at the front to bring them down. The
dogs might be less apt to encounter weapons from people who were fleeing rather
than going into battle, and the dogs may not have been as easily hit by arrows
since they would not have been moving before a backdrop of armed Spaniards. They would have been just as useful in these
circumstances.
I do invite comments to this blog and particularly references to additional sources. Should you not wish to comment publicly, please email me at jensminger@msn.com.
References
Anderson-Córdova, K. F. (2017). Surviving Spanish
conquest: Indian fight, flight, and cultural transformation in Hispaniola and
Puerto Rico. The University of Alabama Press.
Columbus, F. [Fernando Colombo] (1671). Historie de S.D. Fernando Colombo: Nelle quali s'ha particolare, & vera relatione della vits, & de' fatti dell' Ammiraglio D. Christophero Colombo. Venice: Appresso Francesco de' Fraceschi Sanese.
Columbus, F., & Keen, B. (1992). The life of the admiral Christopher Columbus by His Son Ferdinand. New Brunswick: Rutgers University Press.
de Cuneo, M. (1893). Lettera. Savona, 15-28 ottobre 1495. In
Raccolta di documenti e study pubblicati dalla R. Commissione colombiana,
pel quarto centenario dalla scoperta dell’ America (Vol. 2, p. 99).
Ministero della pubblica istruxione, 1892-96.
Deagan, K. A., & Cruxent, J. M. (2002). Columbus’s
outpost among the Taínos: Spain and America at La Isabela, 1493-1498. Yale
University Press.
Denevan, Wi. (1996). Carl Sauer and Native American
Population Size. Latin American Geography, 86(3), 385–397. Figueredo, A. (1978). The Virgin Islands as an Historical
Frontier Between the Tainos and the Caribs. Revista/Review Interamericana,
8(3), 393–399.
Ensminger, J. (2022). From hunters to hell hounds: the dogs of Columbus and transformations of the human-canine relationship in the early Spanish Caribbean. Colonial Latin American Review, 31(3), 354-380.
Figueredo, A. (1978). The Virgin Islands as an historical frontier between the Tainos and the Caribs. Revista/Review Interamericana, 8(3), 393-399.
Floyd, T. S. (1973). The Columbus dynasty in the
Caribbean, 1492-1526 (1st ed.). University of New Mexico Press.
Friede, J., & Keen, B. (Eds.). (1971). Bartolomé de
las Casas in history: Toward an understanding of the man and his work.
Northern Illinois University Press.
Glazier, S. (n.d.). Trade and Warfare in Protohistoric
Trinidad. In Proceedings of the Seventh International Congress for the Study
of Pre-Columbian Cultures of the Lesser Antilles (pp. 279–283). Centre de
Recherches Caraibes.
Guitar, L. (2001). What really happened at Santo Cerro? Origin of the legend of the Virgin de las Mercedes. Caribbean Amerindian Centrelink, Feb. 18. http://indigenouscaribbean.files.wordpress.com/2008/05/guitarsantocerro.pdf.
Heiser, C. B. (1973). Seed to civilization: The story of
man’s food. W. H. Freeman.
Herrera y Tordesillas, A. de. (1601). Historia general de
los hechos de los castellanos en las Islas y Tierra Firme del mar Oceano
(Vol. 1–4). Imprenta de la Real Academia de la Historia.
Hervella, M., San-Juan-Nó, A., Aldasoro-Zabala, A.,
Mariezkurrena, K., Altuna, J., & de-la-Rua, C. (2022). The domestic dog
that lived ∼17,000 years ago in the Lower Magdalenian of Erralla
site (Basque Country): A radiometric and genetic analysis. Journal of
Archaeological Science: Reports, 46, 103706. https://doi.org/10.1016/j.jasrep.2022.103706
Hoffecker, J. F., V.V. Pitulko, & E.Y. Pavlova. (2022).
Beringia and the Settlement of the Western Hemisphere. Bulletin of the St.
Petersburg Department of History, 67(1).
Inigo Abbad y Lasierra. (1866). Historia Geografica,
Civil y Natural. Imprenta y Libreria de Acosta.
Jennings, F. (1975). The invasion of America: Indians,
colonialism, and the cant of conquest. Published for the Institute of Early
American History and Culture by the University of North Carolina Press.
Jennings, F. (1976). The invasion of America: Indians,
colonialism, and the cant of conquest. Norton.
Kroeber, A. L. (1934). Native American Population. American
Anthropologist, 36(1), 1–25.
Kulstad, P. (2008). Concepcion de la Vega 1495-1564: a preliminary look at lifeways in the Americas' first boom town. M.A. thesis, University of Florida.
Kulstad González, P. (2020). Hispaniola—Hell or home?:
Decolonizing grand narratives about intercultural interactions at Concepción de
la Vega (1494-1564). Sidestone Press.
Las Casas, Bartolomé de. 1875–1876. Historia de las Indias. 5 vols. Madrid: Miguel Ginesta.
Martire d’Anghiera, P. (1892). Fuentes históricos sobre
Colón y América (Vol. 1). Imprenta de la S.E. de San Francisco de Sales.
Morison, S.E. (1942). Admiral of the ocean sea: a life of Christopher Columbus. Boston: Little, Brown & Co.
Morison, S. E. (1963). Journals and Other Documents on
the Life and Voyages of Christopher Columbus. The Heritage Press.
Oviedo y Valdés, Gonzalo Fernández de. 1851–1855. Historia general y natural de las Indias
[1535]. 4 vols. Madrid: Real Academia de la Historia.
Pané, F. R. (1999). An Account of the Antiquities of the
Indians. Duke University Press.
Parry, J. H., & Keith, R. G. (Eds.). (1984). New
iberian world: A documentary history of the discovery and settlement of Latin
America to the early 17th century (1st ed, Vol. 2). Times Books : Hector
& Rose.
Perez Fernandez, Jose Maria, and Wilson-Lee, Edward (2021). Hernando Colon's New World of Books: Toward a Cartography of Knowledge. New Haven: Yale University Press.
Rosenblat, A. (1967). La Poblacion de America en 1492:
Viejos y nuevos calculos. Colegio de Mexico.
Sauer, C. O. (1966). The Early Spanish Main.
Cambridge University Press.
Stone, E. W. (2021). The Conquest of Española as a
“Structure of Conjuncture.” Ethnohistory, 68(3), 363–383.
Sued Badillo, J. (Ed.). (2007). General history of the
Caribbean. Volume I, Autochthonous societies. Palgrave Macmillan : UNESCO
Pub.
Tejera, A. (n.d.). La Cruz del Santo Cerro and the Battle of
Vega Real. Boletin Del Archivo General de La Nacion (Santa Dominga), 8(40–41),
101–119.
Tinker, Ti., & Freeland, M. (2008). Thief, Slave Trader,
Murderer: Christopher Columbus and Caribbean Population Decline. Wicazo Sa
Review, 23(1).
Traboulay, David M. (1994). Columbus and Las Casas: The Conquest and Christianization of America, 1492-1566. Lanham, Maryland: University Press of America.
Tyler, S. L. (1988). Two worlds: The Indian encounter
with the European, 1492-1509. University of Utah Press.
Wilson, S. (1997). Surviving European Conquest in the Caribbean.
Revista de Arqueologia Americana, 12, 141–160.
Wilson, S. M. (1990). Hispaniola: Caribbean chiefdoms in
the age of Columbus. University of Alabama Press.






.jpg)








